
CASE NOTES
Review of cases submitted to investigate the cause of cattle deaths in western new south wales (so called 3D syndrome)
Graham Bailey, Cattle Health Coordinator, NSW Department of Primary Industries, Orange and Erika Bunker, Veterinary Pathologist, NSW Department of Primary Industries, Menangle
Posted Flock & Herd April 2015
Introduction
A syndrome with the key signs of drooling and diarrhoea leading to death (3D Syndrome) has been reported by graziers in the Mossgiel, Hay and Ivanhoe area of NSW. Combined losses across all properties where 3D syndrome has been investigated is in the hundreds. At this stage, the cause of 3D syndrome has not been identified. This paper reviews investigations conducted and proposes a case definition for 3D syndrome.
Case reports
Submissions to the NSW Department of Primary Industries (DPI) veterinary laboratories during the period January 2006 to June 2014 were reviewed. Submissions included in the review were those where the attending veterinarian was investigating morbidity/mortality in cattle and nominated on the submission "western cattle deaths" or "3D syndrome". The principle material reviewed was the veterinarian's specimen advice form and the laboratory report which was supplemented with photos, videos and additional case notes if available. In addition, where possible property owners were visited with additional owner details obtained and paddock maps prepared. Where available, histopathology was reviewed.
In the period, a total of 66 submissions were received from 15 properties. Farmers typically reported mortalities in November-December, though in 2014 they extended to January. Investigations commenced during these months in 2006, 2009 and 2013/4 resulted in 17, 16 and 33 laboratory submissions respectively. Submissions were received from 11 properties in a single year of investigation (2006-3; 2009-3; 2013- 5) and 4 properties in two years of investigation (2009 and 2013). Information regarding animals involved was reviewed from the sample advice form supplemented by on farm interviews with 10/15 property owners/managers. Given the extensive nature of the holdings and the fact that deaths often involved young calves, it was not possible to obtain an accurate figure of total losses. However across all properties, losses were in the hundreds with some landholders reporting a high proportion of affected cattle in some but not all mobs of cattle. For example a property had one affected and one unaffected cow and calf mob in 2009 and 2013/4 with >50% mortality in the affected mob in both years. For submissions with young cattle, it was not always possible to determine the ages of the affected animals. For 6 properties (13 submissions), major presenting signs was diarrhoea in calves up to 12 weeks of age with the only other submission from these properties being a stillborn calf with menigoencephalitis with Chlamydia pecorum detected by polymerase chain reaction (PCR).There have been no reports of cattle sold from the 15 properties developing similar disease on the destination properties or cattle in contact on the destination properties developing similar disease. Similarly, there have been no reports of introduced cattle to the 15 properties developing disease at varied prevalence to homebred cattle.
The majority of submissions included sampling a dead animal or a euthanased affected animal (40/66-60% of submissions).The remaining submissions were samples from other animals in the mob as follow up tests, water (3) or insect traps (1).
On affected properties owners have reported: mild illness initially "off colour", prefer to lie down (sternal recumbency). Drooling was regularly observed. Epiphora and stridor was reported in some cases. Diarrhoea was regularly noted with mucus or blood observed in the faeces. As the disease progressed, affected cattle moved to lateral recumbency. Generally there was no or little struggling prior to death though convulsions were reported in some cases. Death generally occurred 1-5 days after first noting sick with nearly all affected animals dying. Cattle have generally been reported to be in good to very good condition. Cattle feel hot and if temperature was measured, were febrile (40-42°C). Affected animals were often reported close to water or in shade.
While some changes have been noted on clinical pathology, no consistent pattern was detected.
Post-mortems were conducted in 40/66(60%) of submissions. There were no consistent changes across all submissions. Where pathology was noted, it was most consistently in the gastrointestinal tract. Particularly in the 2013-4 cases, oesophageal changes were frequently observed. Externally, increased diameter with oedema and occasionally haemorrhages on the serosal surface was noted. When opened, mucosal congestion, haemorrhages and erosions were often seen with an overlying exudate which in severe cases extended the entire length of the oesophagus.
Figure 1: Proximal oesophagus showing erosions that in places coalesce surrounded by congested mucosa.

8 month old steer Photo G Curran

12 month old steer Photo N Gillan
Figure 2: Oesophagus of 5 month old calf showing marked congestion with a mucopurulent exudate

Photo courtesy C Peake
Small and large intestinal congestion, haemorrhage, ulceration with fibrin casts has been observed in some animals.
Figure 3: 6-8 week old calf. Small intestine congested and jejunal lymph nodes appeared enlarged and inflamed. Salmonella enterica serovar Give isolated.

Figure 4: 10-12 week old calf- Caecum with haemorrhagic casts within lumen. Salmonella enterica serovar Anatum isolated.
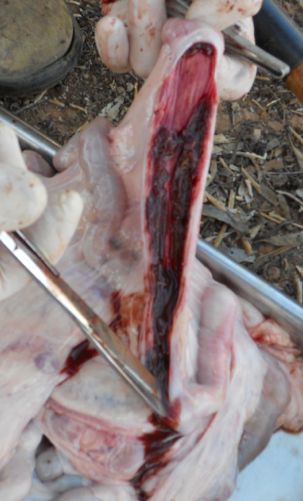
During post-mortems, it has been noted on some occasions that blood clots slowly.
Forty/66 (60%) of submissions included samples from a dead animal for histopathology. Of all organ systems, the alimentary tract was most consistently and most severely affected (with no primary aetiology established in most cases submitted). Within the alimentary tract, oesophagus (submitted routinely with the 2013/14 cases, not in earlier outbreaks so lesions may have been missed) and large intestine were most consistently and most severely affected; in many cases the small intestine was also affected but generally the lesions were not as severe as in the large intestine. While abomasal lesions were seen in only a minority of cases, some of those lesions appeared to be part of the unknown disease process, or sequel of it, showing the feature of vascular damage. Forestomach lesions were rarely seen, however, forestomach was not available for histopathology in most cases and could have been missed. Mouth lesions were noted grossly and histologically one animal. Liver lesions were noted in about half the cases, however, most of them were non-specific degeneration or mild and not significant, rarely bacterial hepatitis or hepatic necrosis.
In the respiratory tract, in rare cases tracheal and/or laryngeal lesions were seen, sometimes together with oesophageal lesions, and of similar severity. Lung lesions were seen in half of the lungs examined histologically, and in the majority of cases a diagnosis of secondary bacterial pneumonia could be established. There was an exception of 2 cases from the Hay area with severe acute haemorrhagic lung lesions.
The spleen was depleted in a bit less than half of spleens examined histologically. There were variable lymph node lesions, mostly non-specific or indicative of drainage of organs with lesions. One case had vascular damage within a lymph node of unknown aetiology.
There was no histopathological evidence of urinary tract involvement. Kidneys were submitted with most cases and generally showed no lesions; only 2 calves had nephritis and one case had a nephropathy suggestive of a toxic aetiology.
Brains were not consistently submitted as there was no evidence of significant neurological signs. A few brains from animals were submitted as some of the animals later in the course of disease developed gait changes. A stillborn calf from a property that later had young calves with diarrhoea had multifocal meningoencephalomyelitis affecting blood vessels and tested PCR positive for Chlamydia pecorum. Additionally, non-suppurative meningoencephalomyelitis and neuritis with vasculitis was seen in 2 calves with neurological signs from a property with no typical 3D syndrome cases; these calves were not considered typical of 3D. One case of hepatic encephalopathy was also considered not typical for 3D.
Muscle lesions were found in 2 cases atypical 3D cases.
Serositis was not a typical finding and seen only in 1 submission in 2009 and 2 submissions from one property in 2013/14.
Tests for a wide range of infectious and toxic aetiologies have been conducted with largely negative results.
Various infectious agents have been detected. Thirty seven faeces and/or intestinal content samples were cultured for Salmonella with Salmonella enterica isolated from 11 submissions with serovars including Typhimurium (3), Adelaide(3), Chester, Singapore, Orion, Havana, Give and Anatum (1 each). Rotavirus was detected in 1/10 submissions.
Bovine viral diarrhoea virus (BVDV) Pestivirus antigen capture ELISA (PACE) and/or BVDV PCR has been conducted in 44 submissions with negative results from 41. In the 3 submissions with positive results, in one submission from 2009, samples suitable for testing were not received from the autopsied animal but 1/3 live cohorts from the same mob tested positive. In 2013, evidence of transient infection in the last 3 months was detected in cohorts from the affected mob in 2 submissions but all autopsied animals from 4 submissions were PACE negative. In April 2014, newborn calves born from the affected mob were PACE (1/5) or PCR (2/5) positive. In addition BVDV serology was performed in 6 submissions from 5 properties. These indicated that recent BVDV infection had occurred in 4 submissions with one submission negative and one submission involving calves with low titres suggestive of colostral transfer of antibody. Thus while there is evidence of BVDV infection on some properties, 3D syndrome is not a result of persistent infection with BVDV.
Bovine Herpes virus (BHV)- specific tests for BHV1 and BHV5 have been performed. PCR and virus isolation when performed have been negative (including a submission where histopathology and inclusions highly suggestive of herpes virus were observed). However BHV infection in some mobs on some properties has occurred as serology for BHV has been positive.
Other endemic viral tests have included bovine malignant catarrh virus, epizootic haemorrhagic disease virus, bovine immunodeficiency virus, bovine leukaemia virus, orbivirus group, paramyxovirus, flavivirus generic, bovine ephemeral fever virus, rabbit haemorrhagic disease virus all with negative results. In addition retrovirus testing has been performed on 2 submissions with sequences of endogenous retroviruses which are present in all cattle detected. These viruses are very unlikely to be the cause of the mortalities.
Specific tests for exotic virus diseases including foot-and-mouth disease and rinderpest have been performed with all tests negative.
In addition to the specific virology tests, virus isolation in cell culture using a wide range of cell types (cattle and insect) known to detect a broad range of different virus families has been performed with no isolates obtained.
Next-generation sequencing (NGS), also known as high-throughput sequencing has been performed on samples from 2 submissions. Nucleic acid from samples from affected cattle was sequenced. Using bioinformatics, transcriptome subtraction techniques were used to exclude nucleic acid known to be of bovine origin. Remaining sequences were then analysed using basic local alignment search tool (BLAST) for similarities to known microbes. A range of bacteria, mainly enteric bacteria were detected but no viral pathogens were detected.
Toxin testing- arsenic testing was performed on 2 submissions with negative results.
Discussion
A syndrome with the key signs of drooling and diarrhoea leading to death (3D Syndrome) has been reported by graziers in the Mossgiel, Hay and Ivanhoe area of NSW. At this stage, the cause of 3D syndrome has not been identified. Investigations are continuing. A mortality survey of all landowners has been conducted in Western NSW has been conducted and a follow up detailed questionnaire is being conducted. The small number of affected properties makes separating risk factors from confounding factors difficult.
Based on this review, 3D syndrome is not caused simply by the presence of a transmissible agent. Reasons include the small number of affected properties despite cases having been observed since 2006, the presence of affected and unaffected mobs on the same property, the absence of reports of cattle moved from the properties having spread the condition elsewhere nor have introduced cattle been reported with higher morbidity and the extensive range of tests for infectious agents that have failed to identify a potential causal agent. It is most likely the disease occurs as a consequence of multiple factors acting together or sequentially. These factors are most likely to include plants within the paddock (but not a straightforward toxicity). Landholders are constantly encouraged to make contact with veterinarians to have animal health problems investigated.
In an attempt to focus investigations, a case definition has been developed. 3D syndrome is a condition occurring in cattle older than 5 months age, in good condition, with the principal clinical signs of drooling and diarrhoea. To date, cases have occurred in the Western and Riverina Local Land Service and while not occurring in all years typically are seen in November-December, though in 2014 they extended to January. Cases have generally ceased following substantial rain. Affected animals deteriorate quickly with death typically occurring around 72 hours after first signs. At autopsy, externally there are no signs of struggling prior to death and the soil around the head is generally wet from drooling. Internally, oesophageal erosions and ulceration and large intestinal reddening and haemorrhage are the principal findings. Small intestines and other organs may have lesions. Histologically oesophagitis, typhlitis and/or colitis are consistent findings.
On properties where 3D syndrome has occurred, cases of diarrhoea in calves up to 3 months of age have also been seen. Calf diarrhoea is caused by a variety of agents and is regarded as a separate disease.
Based on this case definition, 3D syndrome accounted for 12 investigations on 4 properties. In addition, calf diarrhoea accounted for 13 investigations on 7 properties with other endemic diseases accounting for 12 investigations on 9 properties. It was not possible to allocate a category for 6 submissions.
Acknowledgements
Landholders, some of who have lost significant numbers of cattle, have provided assistance to veterinarians conducting investigations on their properties and provided details about their properties. Field veterinarians Greg Curran, Samantha Yorke, Gabe Maurice, Colin Peake, Wayne Gardham, Dermot McNerney and Nigel Gillan conducted autopsies and supplied additional information about the properties and investigations. A number of other veterinary colleagues have provided advice about various aspects of these investigations. The NSW DPI has provided funding for field investigations and laboratory testing.